
Top Chronic Pain Symptoms Veterans Ignore (and Why Documentation Matters)
Your left knee has been giving you trouble since 2019. Not every day. Some weeks it is fine. Then you take a long drive or spend a weekend walking around, and it swells up and you are limping for three days. You mentioned it to your primary care doctor once, maybe two years ago, and she wrote something in the chart. You figure that counts.
It does not count. Not the way you think it does.
Here is the uncomfortable truth about chronic pain claims: the symptoms veterans ignore are exactly the ones that matter most for ratings, and the reason they matter is not the pain itself. It is the paper trail. Without documentation, your pain is a story. The VA wants evidence.
Nearly one in three VA disability claims were not approved in 2025, according to data reported by Military.com. A meaningful portion of those denials came down to a single, fixable problem: not enough detail in the medical record to show what was happening, how severe it was, and what it stopped the veteran from doing.
The Symptoms You Are Dismissing as Normal
Veterans are exceptionally good at normalizing symptoms. It is part of the training. You learn to function through discomfort, to compartmentalize, to keep moving. That skill kept people alive in combat zones. It is actively working against you in the claims process.
Here are the ones I see dismissed most often.
Intermittent joint pain that flares after activity. This is the knee example. The pattern of flare-and-recovery reads to many veterans as evidence that the problem is not that serious. It is actually one of the most documentable patterns you can have. The key is recording each flare, what triggered it, how long it lasted, and what you could not do while it was active.
Morning stiffness that eases after an hour. This is very common in veterans with knee, back, and shoulder issues from carrying gear, repetitive motions, and physical training over years. Veterans tend to treat it as something that just happens when you get older. It is also exactly the kind of thing that shows up on a well-documented pain diary and gets a rater's attention.
Reduced range of motion that you work around. If you cannot fully rotate your shoulder but you have adjusted your movement patterns so you can still function, you have probably convinced yourself the problem is manageable. You are right that it is manageable. You are wrong that it does not count. Functional limitations that you have compensated for are still functional limitations.
Nerve symptoms: tingling, numbness, radiating pain. These are some of the most underreported symptoms among veterans because they come and go and often seem unrelated to anything specific. Sciatica, peripheral neuropathy, radiculopathy in the neck and back: these are common in veterans with spinal conditions and they are routinely under-documented because the sensation is not constant.
Sleep disruption from pain. Veterans do not typically list sleep as a pain symptom. They list it as a sleep problem, if they list it at all. But sleep disruption from chronic pain is a direct functional limitation and it belongs in your record. Document nights when pain kept you from sleeping, how many hours you got, and how you felt the next day.
Fatigue that does not resolve with rest. Chronic inflammation, pain that taxes the nervous system, medications that do not fully manage symptoms: the fatigue that comes with these is real, documentable, and frequently ignored by veterans who figure it is just part of getting older or being out of shape.

Why Undocumented Symptoms Do Not Count
This is where it gets practical.
When a VA rater reviews your claim, they are not asking whether you have pain. They already assume you do. They are asking three specific questions: What is the condition? How severe is it? What can you not do because of it?
A diagnosis answers the first question. It says nothing about the second or third. That is where the gap lives, and that is where the majority of chronic pain claims either get rated lower than they should or get denied entirely.
Here is the problem with relying on memory. Pain is inconsistent. Anyone who lives with it knows this. Some days are worse than others. Some weeks are fine. Your brain, as a coping mechanism, stops recording the details of pain that you have learned to live with. You remember the bad days. You stop remembering the pattern.
When you file a claim months or years after the fact, you are trying to reconstruct a pattern from memory. You remember the bad days clearly. The pattern of how those bad days connected to activity, weather, sleep, stress, and everything else: that pattern is gone. And without it, the story you are telling is incomplete.
A clinician reviewing your chart does not have your context. They have what was written down. If the chart says "chronic knee pain, stable" and nothing else for two years, that is what the rater has to work with. If the chart says "left knee pain, intermittent, exacerbated by prolonged standing and stairs, patient reports swelling on bad days, limits ability to walk more than a quarter mile," that is a completely different picture.
The difference between those two chart entries is not the quality of care you received. It is the documentation habits of the person who wrote them. You can work within that system. You just have to know how.
The Core Problem: Your Brain Stops Recording
There is research behind this pattern. Chronic pain is inconsistent by definition. The brain, as a survival mechanism, downgrades attention to persistent stimuli. Pain that was once impossible to ignore becomes background noise. You adapt. You compensate. You stop noticing.
This is useful for functioning in daily life. It is catastrophic for building a disability record because you lose the very details that make your case compelling.
A pain diary is not about generating sympathy. It is about compensating for the natural tendency of your brain and your memory to stop recording what it has learned to live with. You are not building a story for a jury. You are giving the rater enough specific, consistent, documented information to understand what is actually happening in your body over time.
How to Start a Pain Diary
You do not need a special form. You do not need an app. You need something you will actually use every day, or at least on the days something happens.
A small notebook works fine. A notes app on your phone works fine. The goal is not perfection. It is consistency over time.
Here is the minimum viable format:
Date and activity context. What did you do today? Long drive, physical task at home, yard work, nothing unusual. This matters because the connection between activity and symptom flare is exactly what the VA needs to see.
Pain level on a 0 to 10 scale. Be honest and consistent. The goal is not to look as bad as possible. The goal is to show the pattern.
Symptom description. Where is the pain? What does it feel like? Sharp, dull, burning, aching. Is it localized or radiating?
Functional impact. What could you not do today, or what did you do with difficulty, because of the pain? Be specific. "Could not sleep through the night" is better than "hurt." "Had to cut the walk short at 20 minutes instead of my usual 45" is better than "knee was bad."
Anything that made it better or worse. Rest, ice, medication, weather, position. This builds the pattern over time and shows the rater that you have been paying attention to your own symptoms.
You do not need to do this every single day. If your pain is relatively stable, a few entries per week is fine. When something changes, document that: a new location, a worse flare, something you used to be able to do that you cannot do anymore.
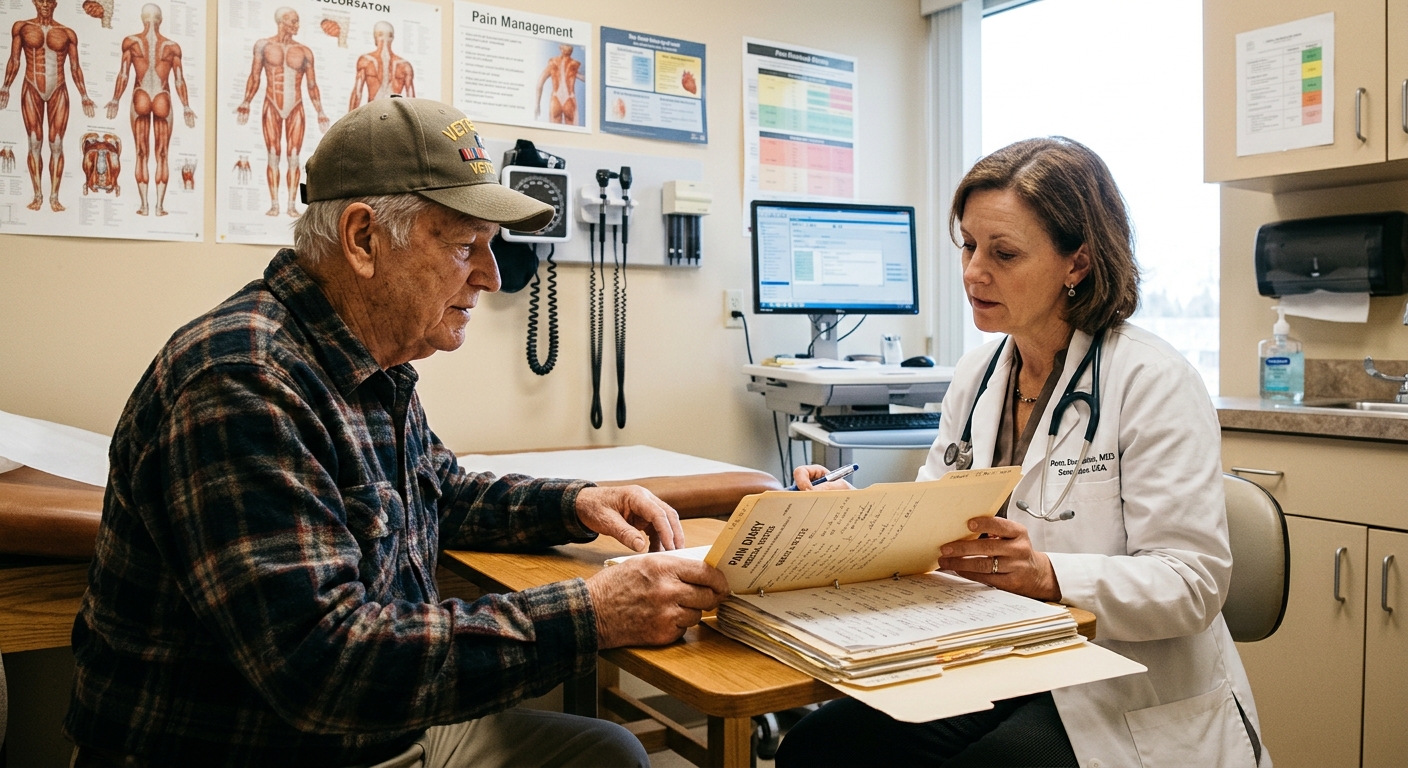
Getting Your Doctor to Take Your Symptoms Seriously
Here is the thing most veterans do not realize: your clinical notes are the primary evidence in your claim. Not imaging. Not the C&P exam, necessarily. Your treating provider's notes are often the most detailed record of your condition over time.
That means the conversation you have with your doctor matters more than you think it does.
Most veterans describe symptoms in terms of coping: they have learned to work around them, push through them, manage them. That framing is honest but it does not generate useful chart notes. "I am managing" does not give a rater anything to work with.
Here is what to say instead:
"This limits me from doing X." Not "this is something I deal with." Not "this has become normal for me." Give the limitation a name. Be specific. "I cannot stand for more than 20 minutes without having to shift my weight or sit down." "I have stopped taking the stairs at work because of my knee." "I sleep in a recliner three or four nights a week because lying flat makes the back pain unbearable."
Ask your provider to document what you tell them, specifically. Most will. A note that says "patient reports chronic left knee pain, intermittent, worsening with activity, currently limits ambulation to approximately 200 yards before requiring rest" is worth significantly more than "chronic knee pain, continues."
If your provider does not ask follow-up questions when you describe a symptom, do not assume that is because the symptom is not important. It is often because they are busy and they need you to give them the detail directly. Come to appointments with a short written list of what you want to discuss. It keeps the conversation focused and it gives your provider something concrete to write down.
The Connection Between Daily Documentation and Your Rating
The VA rates based on functional impairment, not diagnosis. Two veterans can have the same diagnosed condition and receive very different ratings because their documented functional limitations are different. This is not arbitrary. It is the system working as designed. The rating is supposed to reflect how much the condition impairs your ability to function, not just what the condition is called.
Daily documentation builds the picture of your actual functional impairment over time. It shows the rater that the bad days are not isolated incidents but part of a consistent pattern. It shows that you have been tracking this, paying attention, managing as best you can. That kind of record gives a rater the evidence they need to assign an accurate rating.
There is also a practical benefit during C&P exams. When an examiner asks you how your pain affects your daily life, you can say "I documented it" and show them. That is not the same as having your provider's notes, but it demonstrates exactly the kind of consistent self-awareness that examiners look for when they are forming their opinion.
What to Track When You Are Unsure What Matters
If you are starting from zero documentation, it can feel overwhelming to figure out what to track. Here is a useful heuristic: track anything that changes, anything that limits you, and anything you have started avoiding because of pain.
Avoidance is a signal. If you have stopped doing something you used to do because of pain, that is data. It is also one of the most compelling types of data for a rating because it shows functional change over time, not just a static snapshot.
The things veterans most commonly start avoiding when pain progresses: stairs, long walks, standing in place, kneeling or crouching, driving long distances, lifting heavy objects, sleeping in a bed instead of a chair, social activities that involve being on your feet, exercise or physical activities you used to do regularly.
Any of those changes, documented with dates and specificity, is useful evidence.
Bottom Line
Chronic pain claims fail not because the veteran is not in pain, but because the paper trail does not show it clearly enough. Your brain stops recording what it has learned to live with. That is normal. It is also the exact gap that a pain diary fills.
You do not need perfect documentation. You need consistent, specific, honest documentation over time. Dates. Pain levels. What triggered it. What you could not do. What you have stopped doing. That is the data set that tells your story when you cannot tell it yourself from memory.
The discipline you already have from service, the one that lets you push through discomfort and keep functioning: redirect it for five minutes a day toward writing something down. That five minutes is doing more for your claim than another year of quietly managing on your own.
If you need a starting template, Command.ai has a pain diary resource built specifically for veterans navigating the claims process.
Share this article
Help others discover this content
Related Articles
World Mental Health Day, Every Day: A Year-Round Support Plan for Veterans
One awareness day a year is not a mental health strategy. If you are a veteran who wants actual, sustained support, here is what a real year-round plan looks like — with specific resources, what they cost (free), and how to stay consistent when motivation disappears.
Nexus Letters for Skin Conditions: What VA Reviewers Need to See
Skin conditions are one of the most under-claimed and most denied categories in the VA system. A strong nexus letter changes everything. Here is what it needs to say and how to get one that actually works.
Depression in Veterans: Evaluation, Documentation, and Next Steps
Depression hits different after service. Here is how the VA rates it, how to document your symptoms for a claim, and what treatment options are actually available to you right now.